Q. What is "Menarche"?
A. The time of a girl's first menstruation.
Q. When do girls have their first period?
A. Everyone reaches puberty at a different age, but the average is about age 12-15 and will continue to about the age ot 45-50 If you're concerned about not having your period, ask your mother how old she was when she first got hers. There have been many cases where the female was age 18 before her first period. This is a little bit outside of what is concidered normal though. If you have not started to menstruate before age 16, you may want to ask your doctor about it. If you are concerned, ask your doctor. The average menstrual cycle is 28 days, however only a very small percentage of cycles are exactly 28 days, most cycles range from 25-36 days.
Q. What is a "Menstrual Cycle"?
A. The time from the first day of one "period" to the first day of the next "period"; a repeating pattern of fertility and infertility.
Q. What exactly happens when a woman "Ovulates"?
A. I think the best way for most people to understand this would be to show you:
Ovulation actually begins in your head. The Pituitary Gland, located at the base of the brain, produces hormones that enable the Ovaries to begin Ovulation.
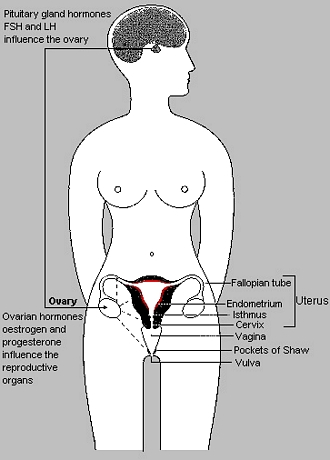
A Follicle, inside of an Ovary, erupts; releasing and egg into the Oviduct (Fallopian Tube).
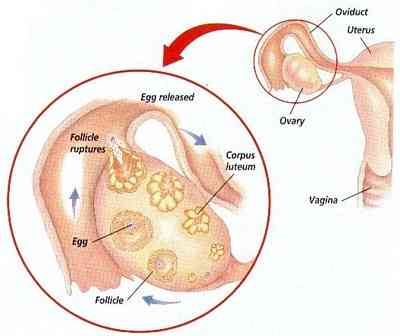
Q. Are there different phases to a menstrual cycle?
A. Yes, the menstrual cycle can be divided into three phases:
the follicular (proliferative) phase
the ovulatory phase
the luteal (secretory) phase
The follicular phase begins with the first day of menses (menstrual flow) and continues to approximately day 13 or 14 when ovulation takes place. During the follicular phase, FSH and LH are slowly rising in preparation for the LH surge (very high level of LH) at the time of ovulation. FSH is stimulating the growth of follicles in the ovary. Estrogen and progesterone are relatively low throughout this time but slowly begin to rise toward the end of this phase. Estrogen, and progesterone to a lesser degree, are steroid hormones produced by cells of the developing ovarian follicle. Estrogen causes the endometrium to increase in thickness and vascularization (i.e.blood supply). At the end of the proliferative (follicular) phase, the endometrium is 2-3 mm thick and the glands are straight tubules with narrow lumens.
Q. Why do I bleed?
A. The blood vessals in the walls of the Uterus become enlarged and finally break through, causing blood to slowly flow. The bood will flow down through the Uterus and out of the Vagina. This happens inconjunction with Ovulation.
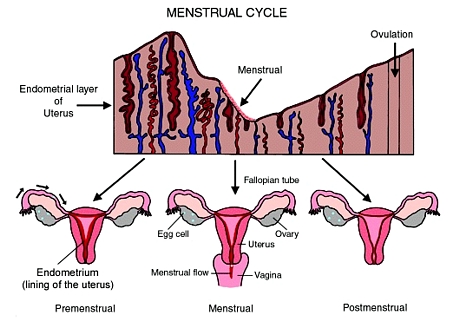
Q. What can I do about cramps?
A. well, there are LOTs of things that you can try, but you probably wont be able to get rid of the cramps completley. There are many over-the-counter medicines that do help many women. Some work well for others and some dont. I will let you choose those for yourself. Here is a small list of what I recommend to try first. They are all natural:
- Increase exercise. This will improve blood and oxygen circulation throughout the body, including the pelvis.
- Eat lots of fresh vegetables, whole grains (especially if you experience constipation or indigestion), nuts, seeds and fruit.
- Meditate, get a massage.
- Have an orgasm (alone or with a partner).
- Drink ginger root tea (especially if you experience fatigue).
- Avoid red meat, refined sugars, milk, and fatty foods
- Avoid caffeine. It constricts blood vessels and increases tension.
- Put cayenne pepper on food. It is a vasodilator and improves circulation.
- Try not using tampons. Many women find tampons increase cramping. and don't select an IUD (intrauterine device) as your birth control method.
- Breathe deeply, relax, notice where you hold tension in your body and let it go.
- Take time for yourself!
Q. What is a "Period"?
A. simple definition: The days during menstruation. (normally 3-6 days)
Q. Is there really a "Fertile Period"?
A. Yes, A woman's fertile period during her menstrual cycle, on average, lasts about nine days: seven days before ovulation (the release of the egg), the day of ovulation, and the day after ovulation. After this, chances of conception decrease quickly, as the egg has a short life-span of about 24 hours.
Q. Can I swim when I have my period?
A. Sure, use a tampon. If you don't know how to use one there are very good instructions on the info sheet inside all boxes.
Q. When having a Pap smear test during a menstrual cycle, can it
A. Yes, You're right: Females don't usually have Pap tests done during their periods. Menstruation does not cause abnormal Pap smear results but, menstrual blood makes abnormal cervical cells much more difficult to see. It is recommended that women schedule a Pap test between ten and twenty days following the start of their periods.
Q. Will masturbating affect my period?
A. Masturbating will not have any effect on your cycle. Any form of sexual activity can bring your menstrual cycle earlier, and for some women ease menstrual cramps, because your body relaxes during sexual activity, and during orgasm, your uterus may experience some contractions. Your menstrual cycle is controlled by hormones that work in rythm every single month.
Q. Will I lose my virginity if I use tampons?
A. No You will not lose your virginity. You are still a virgin if you have not had sexual intercourse. You have nothing to worry about because a virgin is someone who has never had sexual intercourse.
Q. Can I have sex while I have my period? I use tampons, what do I do about that?
A. As long as both of you are comfortable about having sex during your period then of course you can. Since you're a tampon user, remember to remove the tampon before having sex. Or you can use pads around that time.
Q. How often should I change my pad/tampon?
A. Sanitary napkins (pads) should be changed as often as necessary, before the pad is soaked with menstrual flow. Each woman decides for herself what is comfortable. Tampons should be changed often (at least every 4-8 hours). Make sure that you use the lowest absorbency of tampon needed for your flow. For example, do not use super absorbency on the lightest day of your period. This can put you at risk for toxic shock syndrome (TSS). TSS is a rare but potentially deadly disease. Women under 30, especially teenagers, are at a higher risk for TSS. Using any kind of tampon - cotton or rayon of any absorbency - puts a woman at greater risk for TSS than using menstrual pads. The risk of TSS can be lessened or avoided by not using tampons, or by alternating between tampons and pads during your period.
The Food and Drug Administration (FDA) recommends the following tips to help avoid tampon problems:
-
Follow package directions for insertion.
-
Choose the lowest absorbency for your flow.
-
Change your tampon at least every 4 to 8 hours.
-
Consider alternating pads with tampons.
-
Know the warning signs of toxic shock syndrome (see below).
-
Don't use tampons between periods.
If you experience any of the following symptoms while you are menstruating and using tampons, you should contact your health care provider immediately:
Q. What kinds of problems do women have with their periods?
A. Women can have various kinds of problems with their periods, including pain, heavy bleeding, and skipped periods.
-
Amenorrhea - the lack of a menstrual period. This term is used to describe the absence of a period in young women who haven't started menstruating by age 16, or the absence of a period in women who used to have a regular period. Causes of amenorrhea include pregnancy, breastfeeding, and extreme weight loss caused by serious illness, eating disorders, excessive exercising, or stress. Hormonal problems (involving the pituitary, thyroid, ovary, or adrenal glands) or problems with the reproductive organs may be involved.
-
Dysmenorrhea - painful periods, including severe menstrual cramps. In younger women, there is often no known disease or condition associated with the pain. A hormone called prostaglandin is responsible for the symptoms. Some pain medicines available over the counter, such as ibuprofen, can help with these symptoms. Sometimes a disease or condition, such as uterine fibroids or endometriosis, causes the pain. Treatment depends on what is causing the problem and how severe it is.
-
Abnormal uterine bleeding-vaginal bleeding that is different from normal menstrual periods. It includes very heavy bleeding or unusually long periods (also called menorrhagia), periods too close together, and bleeding between periods. In adolescents and women approaching menopause, hormone imbalance problems often cause menorrhagia along with irregular cycles. Sometimes this is called dysfunctional uterine bleeding (DUB). Other causes of abnormal bleeding include uterine fibroids and polyps. Treatment for abnormal bleeding depends on the cause.
Q. When should I see a doctor about my period?
A. You should consult your doctor for any of the following:
-
If you have not started menstruating by the age of 16.
-
If your period has suddenly stopped.
-
If you are bleeding for more days than usual.
-
If you are bleeding excessively.
-
If you suddenly feel sick after using tampons.
-
If you bleed between periods (more than just a few drops).
-
If you have severe pain during your period.
Q. How do I Talk to my Doctor or Nurse about all this stuff?
Waiting in your doctor’s office can be a nerve-wracking experience. As you flip through old magazines in the waiting room, you might worry about what’s wrong or become aggravated about getting behind schedule. Then, when you see your doctor, the visit seems to fly by, leaving only a few minutes for you to explain your symptoms and concerns. Later that night, you remember something you forgot to mention and wonder if it matters. Knowing how to talk to your doctor or other members of your health care team will help you get the information you need, when you need it, especially when visits are oftentimes short. Here are some tips for talking with your doctor.
- Make a list of concerns and questions to take to your visit with your doctor. While you’re waiting to be seen, use the time to review your list and organize your thoughts. You can share the list with your doctor.
- Describe your symptoms clearly and briefly. Say when they started, how they make you feel, what triggers them, and what you’ve done to feel better.
- Tell your doctor what prescription and over-the-counter medicines, vitamins, herbal products, and other supplements you’re taking. Be honest about your diet, physical activity, smoking, alcohol or drug use, and sexual history — withholding information can be harmful! Describe allergies to drugs, foods, or other things. Don’t forget to mention if you are being treated by other doctors, including mental health professionals.
- Don’t feel embarrassed about discussing sensitive topics. Chances are, your doctor has heard it before! Don’t leave something out because you’re worried about taking up too much time. Be sure to have all of your concerns addressed before you leave.
- If your doctor orders tests, be sure to ask how to find out about results and how long it takes to get them. Get instructions for what you need to do to get ready for the test(s) and find out about any dangers or side effects with the test(s).
- If you are diagnosed with a condition, ask your doctor how you can learn more about it, including what caused it, if it is permanent, and if there are lifestyle changes you can make to help yourself feel better. Be sure to ask about all of the options for treatment, and how you can find out more information about
treatment options.
- When you are given medicine and other treatments, ask your doctor about them. Ask how long treatment will last, if it has any side effects, how much it will cost, and if it is covered by insurance. Make sure you understand how to take your medicine; what to do if you miss a dose; if there are any foods, drugs, or activities you should avoid when taking the medicine; and if there is a generic brand available at a lower price (you can also ask your pharmacist about this).
- Understand everything before you leave your visit. If you don’t understand something, ask to have it explained again.
- Bring a family member or trusted friend with you to your visit. That person can take notes, offer moral support, and help you remember what was discussed. You can also have that person ask questions as well.
- This information was provided by http://www.4woman.org
Q. Is there a list of common tests done just for women?
A. yes, there is. Here is a list of the most common Screening and Diagnostic Tests:
| Angiogram |
Exam of your blood vessels using x-rays. The doctor inserts a small tube into the blood vessel and injects dye to see the vessels in the x-ray. |
| Barium enema |
A lubricated enema tube is gently inserted into your rectum. Barium flows into your colon. An x-ray is taken of the large intestines. |
| Biopsy |
Removal of a small piece of tissue to check for health problems. There are different types of biopsies. |
| Blood test |
Blood is taken from a vein in the inside elbow or back of the hand to test for a health problem. |
| Bone mineral density test (BMD) |
X-rays of the bones are tested for osteoporosis, or weakening of the bones. |
| Bronchoscopy |
Exam of the lungs. A bronchoscope, or flexible tube, is put through the nose or mouth and into your windpipe (trachea). |
| Clinical breast exam (CBE) |
A doctor looks at the breasts and underarm areas to find lumps or other problems. |
| Chest x-ray |
An x-ray of the chest, lungs, heart, large arteries, ribs, and diaphragm. |
| Colonoscopy |
A flexible tube is put into the colon through the anus to see the colon. |
| Computed tomographic (CT or CAT) scan |
The patient lies on a table and x-rays of the body are taken from different angles. Sometimes, a fluid is used to highlight parts of the body in the scan. |
| Echocardiogram |
An instrument (that looks like a microphone) is placed on the chest. It uses sound waves to create a moving picture of the heart. A picture appears on a TV screen, and the heart can be seen in different ways. |
| Electroencephalogram (EEG) |
Measures the electrical activity of the brain, using electrodes that are put on the patient’s scalp. Sometimes patients sleep during the test. |
| Electrocardiogram (EKG or ECG) |
Records the electrical activity of the heart, using electrodes placed on the arms, legs, and chest. |
| Exercise stress test |
Electrodes are placed on the chest, arms, and legs to record the heart’s activity. A blood pressure cuff is placed around the arm and is inflated every few minutes. Heart rate and blood pressure are taken before exercise starts. The patient walks on a treadmill or pedals a stationary bicycle. The pace of the treadmill is increased. The response of the heart is monitored. The test continues until target heart rate is reached. Monitoring continues after exercise for 10 to 15 minutes or until the heart rate returns to normal. |
| Fecal occult blood test (FOBT) |
Detects hidden blood in a bowel movement. There are two types: the smear test and flushable reagent pads. |
| Laparoscopy |
A small tube with a camera is inserted into the abdomen through a small cut in or just below the belly-button to see inside the abdomen and pelvis. Other instruments can be inserted in the small cut as well. It is used for both diagnosing and treating problems inside the belly. |
| Magnetic resonance imaging (MRI) |
The patient lies on a table which slides into a large tunnel-like tube within a scanner. Small coils may be placed around the head, arm, leg, or to other areas. Powerful magnets and radio waves create pictures of the body. |
| Mammogram |
One breast at a time is rested on a flat surface that contains an x-ray plate. A device presses firmly against the breast. An x-ray is taken to show a picture of the breast. |
| Medical history |
The doctor or nurse talks to the patient about current and past illnesses, surgeries, pregnancies, medications, allergies, use of alternative therapies, vitamins and supplements, diet, alcohol and drug use, physical activity, and family history of diseases. |
| Pap test |
The nurse or doctor uses a small brush to take cells from the cervix (opening of the uterus) to look at under a microscope in a lab. |
| Pelvic exam |
A doctor or nurse asks about the patient’s health and looks at the vaginal area. The doctor or nurse checks the tubes, ovaries, and uterus by putting two gloved fingers inside the vagina. With the other hand, the doctor or nurse will feel from the outside for any lumps or tenderness. |
| Physical exam |
The doctor or nurse will test for diseases, assess your risk of future medical problems, encourage a healthy lifestyle, and update your vaccinations. |
| Positron emission tomography (PET) scan |
The patient is injected with a radioactive substance, like glucose. A scanner detects scan any cancerous areas in the body. Cancerous tissue absorbs more of the substance and looks brighter in images than normal tissue. |
| Sigmoidoscopy |
The sigmoidoscope is a small camera attached to a flexible tube. This tube, about 20 inches long, is gently inserted into the colon. As the tube is slowly removed, the lining of the bowel is examined. |
| Spirometry |
The patient breathes into a mouthpiece that is connected to an instrument called a spirometer. The spirometer records the amount and the rate of air that is breathed in and out over a specified time. It measures how well the lungs exhale. |
| Ultrasound |
A clear gel is put onto the skin over the area being examined. An instrument is then moved over that area. The machine sends out sound waves, which reflect off the body. A computer receives these waves and uses them to create pictures of the body.
Provided by http://www.4woman.org |
|